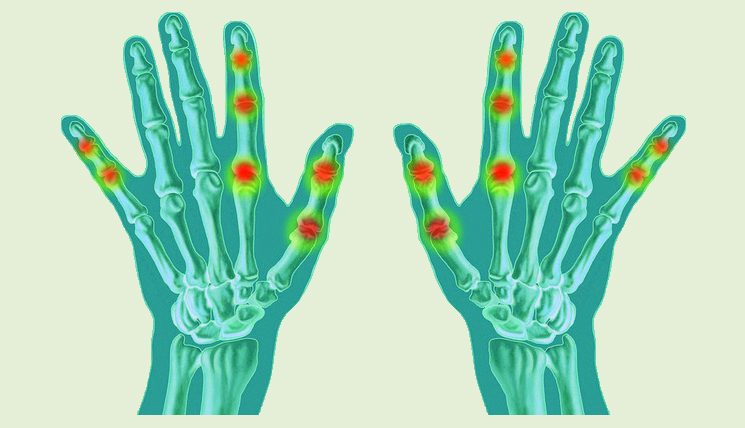
Sie verursachen ganz ähnliche Symptome, haben aber völlig unterschiedliche Ursachen: die Chikungunya-Virusinfektion und die Rheumatoide Arthritis.
Das Chikungunya-Virus (CHIKV) wird durch Stechmücken auf den Menschen übertragen, speziell durch die Gelbfiebermücke (Aedes aegypti) und die Asiatische Tigermücke (Aedes albopictus). Die Insekten sind wahre Virenschleudern, können sie doch auch die Erreger des Dengue-, Gelb-, und West-Nil-Fiebers übertragen. Zuerst entdeckt wurde das CHIKV Anfang der 50er Jahre in Tansania, später traten auch erste Fälle im Westen des Kontinents sowie in Indien und Südostasien auf. In den letzten Jahren haben sich die Stechmücken und somit auch das Virus u.a. in der Karibik und in Südamerika besorgniserregend schnell ausgebreitet.
Eine Infektion mit CHIKV führt gewöhnlich nach einer Inkubationszeit von 3 bis 7 Tagen zu einem plötzlichen Fieberausbruch, starken Kopfschmerzen sowie geschwollenen und extrem berührungsempfindlichen Gelenken. Oftmals treten diese Symptome zusammen mit einem fleckigen Hautausschlag (Exanthem) oder einer generalisierten Hautrötung auf. Bei den meisten Betroffenen klingt die Krankheit von selbst wieder ab, bleibende Schäden und Komplikationen sind eher selten. Bis zu 10% der Patienten leiden jedoch noch über Monate oder in seltenen Fällen sogar über Jahre an den schmerzenden Gelenkentzündungen, welche die Bewegungsfreiheit stark einschränken. Da sich die Betroffenen kaum aufrecht halten können, wurde das Fieber „Chikungunya“ genannt – einem Wort aus der Sprache der Makonde (ethnische Bevölkerungsgruppe aus Ostafrika), das so viel wie „gekrümmt Gehender“ bedeutet. Ganz ähnlich wie bei der Rheumatoiden Arthritis (RA) tritt diese sogenannte Chikungunya-assoziierte Arthritis symmetrisch in den Gelenken der linken und rechten Körperhälfte auf.
Im Gegensatz zu der Tropeninfektion handelt es sich bei der RA jedoch um eine Autoimmunerkrankung, bei der die Entzündung und Schädigung der Gelenke durch eine Immunabwehr-Reaktion gegenüber körpereigenen Strukturen ausgelöst wird. Eine Diagnose der RA erfolgt anhand festgelegter Klassifikationskriterien des American College of Rheumatology/European League Against Rheumatism (ACR/EULAR), die folgende Faktoren berücksichtigen: Anzahl und Größe der betroffenen Gelenke, Dauer der Entzündung, Serologie (Nachweis von Rheumafaktoren und Autoantikörpern gegen cyclische citrullinierte Peptide (ACPA) im Serum) sowie allgemeine Entzündungsmarker. Trifft eine definierte Anzahl dieser Kriterien bei einem Patienten zu und gibt es keine Hinweise auf eine andere Ursache für die Beschwerden, so gilt die Diagnose der RA als sicher. Wie sich in einer im Mai veröffentlichten US-amerikanischen Studie gezeigt hat, können die Kriterien aber auch von der Chikungunya-assoziierten Arthritis ausreichend erfüllt werden. Miner et al. haben gezeigt, dass 8 von 10 Patienten mit Gelenkentzündungen, bei denen eine CHIKV-Infektion bereits diagnostiziert war, gemäß der ACR/EULAR-Kriterien (2010) als (seronegative) RA-Patienten eingestuft worden wären, wenn es keine Informationen über ihren Aufenthalt auf Haiti gegeben hätte – und das, obwohl keine RA-spezifischen Autoantikörper oder Rheumafaktoren in den entnommen Blutproben nachgewiesen werden konnten. Was also zunächst aussieht wie eine (seronegative) RA, könnte in manchen Fällen tatsächlich eine Infektion mit dem CHIKV sein.
Klarheit darüber können die weiteren Symptome, eine Klärung kürzlich vergangener Aufenthalte in gefährdeten Regionen und zusätzliche Blutuntersuchungen schaffen. Ab dem 6. Tag nach dem Einsetzen der ersten Beschwerden sind mithilfe serologischer Verfahren (ELISA, Indirekte Immunfluoreszenztests) in der Regel spezifische Antikörper (IgM, IgG) gegen das Virus im Serum nachweisbar. Wer eine Infektion dann schließlich überstanden hat, ist vermutlich den Rest seines Lebens gegen CHIKV immun.